This is the third of a five-part newsletter series that discusses etiology, risk factors, diagnosis, prevention, and treatment of peri-implant disease.
Multiple risk factors have been associated with peri-implant diseases.
- Poor oral hygiene
- Lack of keratinized gingiva
- Smoking
- History of periodontitis
- Parafunctional habits
- Systemic diseases and medications
- Restorative factors
- Retained cement
- Implant surface conditions
These are reviewed below:
Oral Hygiene
Poor oral hygiene is an obvious and major risk factor for peri-implant diseases. One study showed that implant sites that have difficult access for adequate oral hygiene exhibited greater amount of plaque accumulation, and peri-implantitis developed in 48% of those implants; as compared to more accessible plaque control sites developing peri-implantitis in 4% of the sites. Another study showed that in patients with peri-implant mucositis, 44% of those implants developed peri-implantitis within 5 years. In patients without peri-implant mucositis, 18% developed peri-implantitis. Other factors such as poor prosthetic design and exposed roughened implant surfaces lead to greater plaque accumulation and retention resulting in the progression of peri-implantitis.
Lack of Keratinized Gingiva
The presence of adequate attached gingiva around implants helps to maintain the health of the soft and hard tissue. Lack of attached gingiva appears to be associated with increased inflammation, difficulty in plaque control, and increased plaque accumulation, recession, and bone loss.
Smoking
Smoking is often the most cited risk factor for peri-implantitis. Studies show implant failures ranging from 35% to 70% when smoking before or after implant placement. Smoking’s effect on the host response is well-established. Even greater risk has been shown with smokers with a history of periodontal disease.
History of Periodontal Disease
Patients with a history of chronic periodontal disease are more susceptible to developing peri-implantitis (28%) than healthy patients (6%). Periodontal pockets can be a reservoir for the transfer of periodontal pathogens to an adjacent implant site, resulting in peri-implantitis.
Parafunctional Habits
Bruxism is considered a major risk factor for peri-implant diseases. Lateral forces resulting from parafunctional habits can lead to non-integration of an implant in the early phase of placement, implant fracture, and bone loss around the implant. The excessive non-axial forces are thought to create a resorptive bone remodeling effect resulting in bone loss at the implant surface. Teeth maintain a periodontal ligament, which protects the teeth through proprioception and allowing minor movement. Dental implants do not have a periodontal ligament and thus lack proprioception. During treatment planning and treatment phases of dental implants, the principles of occlusion and the controlling of bruxism must be closely followed to prevent implant overloading.
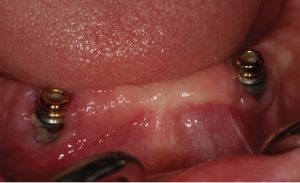
Dental implant with minimal keratinized gingiva, thus making this a greater risk of developing peri-implantitis
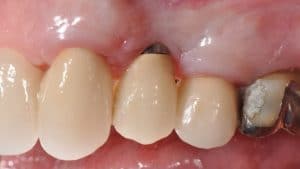
Plaque accumulation around an implant, causing peri-implantitis

 Dr. Sakamoto
Dr. Sakamoto
 Dr. Mannava
Dr. Mannava
 Our Team
Our Team
 FIRST VISIT
FIRST VISIT
 PATIENT FORMS
PATIENT FORMS
 DENTAL INSURANCE
DENTAL INSURANCE
 POST-OP INSTRUCTIONS
POST-OP INSTRUCTIONS